A new McKinsey Health Institute report issues a clear warning: if we do not transform the current approach to healthcare systems, by 2050 we will live longer, but spend more time ill. And that is not only a clinical problem, but also an economic one.
The study, The health of nations: stronger health, stronger economies, concludes that, by expanding access to proven, cost-effective health interventions, each person could gain up to nine extra years of healthy life by 2050. The aggregate impact would be monumental: an estimated boost of 12.5 trillion dollars a year to the global economy, equivalent to about 7 % of world GDP.
The question is whether systems are ready - and willing - to change.
We live longer, but get sick longer
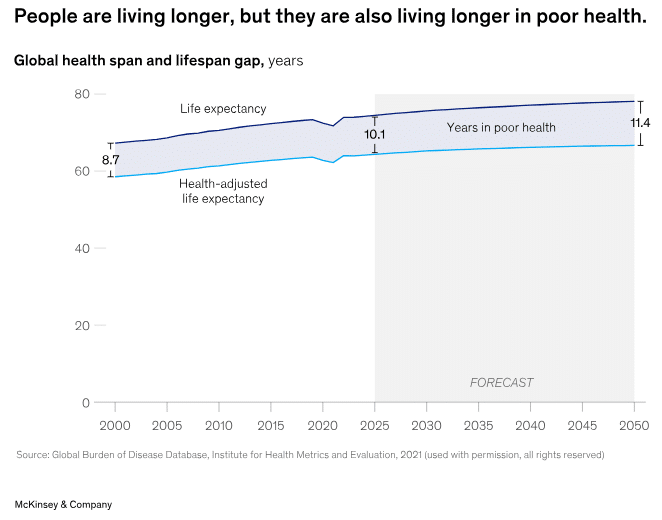
Average life expectancy worldwide will reach 78 years in 2050, eleven more than half a century ago. However, the really relevant fact is another: the time lived with illness continues to increase.
- In 2000, the average number of years lived with illness was 8.7.
- In 2025, it rises to 10.2
- In 2050, it is projected to reach 11.4 years.
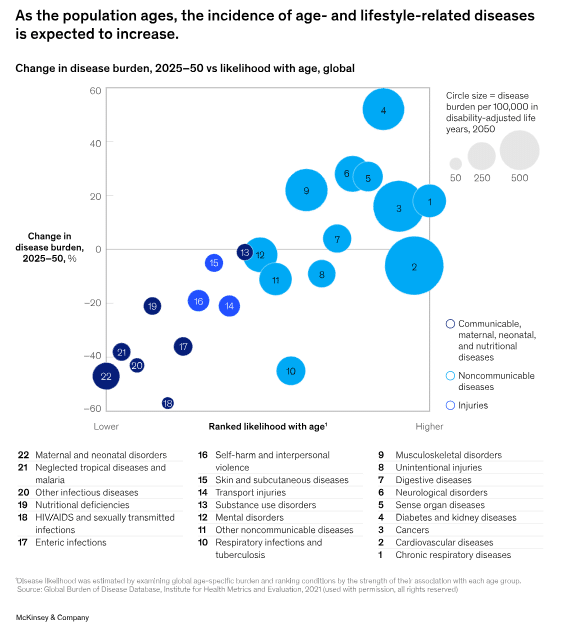
At the same time, population ageing and the increase in non-communicable diseases - cardiovascular disease, diabetes, cancer, mental disorders - are chronifying healthcare spending and reducing productivity.
More older people, less working-age population and fewer total hours worked: the direct consequence is a structural slowdown in GDP per capita growth. The paradox is obvious: we are making progress in longevity, but not in healthspan (years lived in good health).
Prevention: the forgotten investment
One of the most critical findings of the report is that the majority of countries allocate less than 2 % of its health budget to prevention.
Institutional inertia, fragmented systems and fiscal pressures maintain a model focused on treating disease, not preventing it.
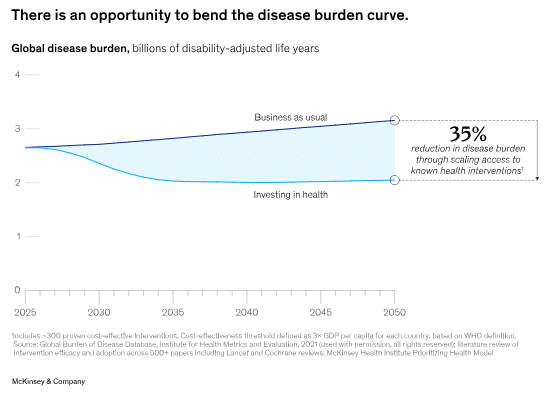
However, the economic evidence is compelling. Scaling up proven preventive interventions could:
- Prevent 33 million premature deaths
- Reducing more than 461 million years lived in ill-health
- Generate an estimated four times return on investment
A simple example: expanding global access to hypertension treatment would cost less than $5 per person per year and prevent millions of deaths over 25 years. Prevention is not ideology; it is economic mathematics.
The role of the wellness sector: opportunity and contradiction
The wellness industry has embraced the longevity discourse, but the report suggests that the true potential for health expansion remains underexploited.
There is a disconnect between:
- Premium innovations aimed at affluent consumers
- Basic, scalable, high-impact population-based interventions
Longevity cannot be solely an aspirational commodity. Without democratising access to cost-effective interventions - structured physical activity, adequate nutrition, metabolic control, mental health - the systemic impact will be limited.
Three axes to change the trajectory
The report identifies three key lines of action.
1. Aligning financial incentives towards prevention
Funders - public and private - must reward long-term investments in population health.
Organisations such as the World Health Organization underline that prevention is one of the highest return on investment in a health system. Even in the treatment of obesity, where drugs such as GLP-1 agonists have gained prominence, physical activity remains essential.
Without structural incentives, the system will continue to reward late intervention rather than early prevention.
2. Integrating health and economic development
Health is not just a health ministry issue.
School feeding programmes improve attendance and academic performance. Safe water infrastructure reduces disease. Active urban environments reduce cardiovascular risk.
Countries that integrate health investments with education, urban and social policies achieve more sustainable growth.
Incorporating health impact assessments into national planning could be a critical tool.
3. Improve efficiency and expenditure management
It is not just about spending more, but about spending better.
The use of artificial intelligence, digital infrastructures and data analytics can optimise real-time resource allocation, improve adherence and scale interventions with greater return.
The key is to prioritise actions that combine high health impact with high social returns.
The deterioration of healthspan is not inevitable. But maintaining the status quo is, if structural changes are not introduced.
In an ageing world, the real wealth will not be to live longer, but to maintain functional, cognitive and productive capacity for longer.
The equation is clear: more health means more economic growth.
The question is not whether we can afford to invest in prevention. The question is how much it will cost us not to do so.






